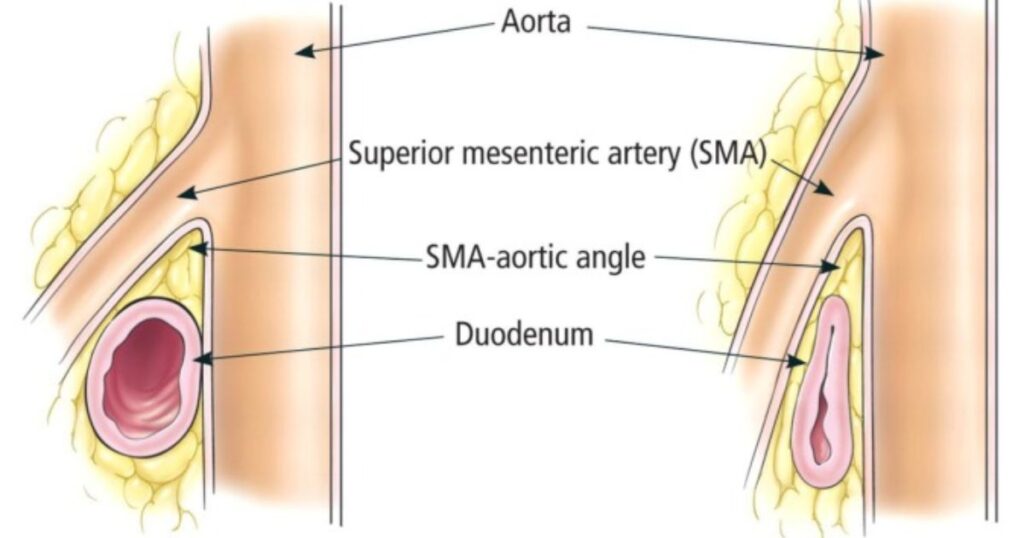
Superior Mesenteric Artery Syndrome (SMAS) is a rare but serious digestive disorder that affects the upper part of the small intestine. It happens when the superior mesenteric artery compresses the duodenum, creating a gastrointestinal blockage.
This can lead to difficulties with digestion, nutrient absorption, and may put someone at a malnutrition risk. Patients often experience abdominal pain, nausea and vomiting, and early satiety and bloating, especially after meals. While SMAS is uncommon, it can be life-threatening if left untreated. Understanding the causes, symptoms, and treatment options is vital for patients, caregivers, and healthcare providers in the USA.
The SMAS anatomy plays a crucial role in this disorder. Normally, the mesenteric fat pad cushions the superior mesenteric artery, keeping the angle wide enough for food to pass through the duodenum. When this fat pad shrinks due to rapid weight loss, bariatric surgery complications, or other causes, the duodenum becomes pinched.
This leads to gastric outlet obstruction and impaired small intestine function, affecting the body’s ability to absorb nutrients properly. Early diagnosis and intervention are key to avoiding severe outcomes like aspiration pneumonia or hypovolemic shock.
What Is Superior Mesenteric Artery (SMA) Syndrome?
Superior Mesenteric Artery Syndrome is a condition where the superior mesenteric artery compresses the duodenum, creating a blockage in the upper small intestine. This obstruction slows down digestion and often causes abdominal pain, nausea and vomiting, and discomfort after eating. In some cases, patients experience early satiety and bloating, which makes it hard to consume enough calories. SMAS affects the digestive system anatomy and can lead to serious life-threatening complications if untreated.
The SMAS face and overall presentation can vary widely. Some patients experience mild symptoms for years, while others develop rapid weight loss, dehydration, and severe gastrointestinal obstruction. The condition may arise after bariatric surgery complications, spinal injuries, or prolonged illness. Understanding the small intestine function and how the mesenteric fat pad protects the duodenum is essential for recognizing SMAS early. Without proper treatment, patients are at risk of malnutrition, electrolyte imbalance, and chronic digestive issues.
How Does SMAS Affect Digestion?
When the duodenum is compressed, food cannot move normally through the small intestine. This creates gastrointestinal blockage, slows nutrient absorption, and increases the risk of malnutrition. Patients often report feeling full quickly and discomfort immediately after meals, which can affect daily life and overall health. The obstruction can worsen without intervention, leading to severe gastrointestinal obstruction that requires urgent SMAS surgery.
Causes and Risk Factors
The main SMAS causes involve the loss of the mesenteric fat pad, which normally maintains the angle between the superior mesenteric artery and the aorta. Rapid weight loss, malnutrition, or chronic illnesses like cancer or eating disorders can trigger this. Patients recovering from bariatric surgery complications, spinal trauma, or prolonged bed rest are also at higher risk. Some genetic factors may contribute, but further studies are needed.
Other risk factors include trauma, burns, or chronic illness that decreases fat tissue around the duodenum. Individuals who have lost weight quickly may notice abdominal pain, early satiety and bloating, and persistent nausea. Understanding the digestive system anatomy and how fat cushions the duodenum helps explain why certain patients are more susceptible. Medical history evaluation and careful monitoring are crucial for preventing severe consequences.
Symptoms and Complications
Patients with SMAS often experience abdominal pain, nausea and vomiting, early satiety, and bloating. These symptoms usually worsen after meals and can lead to anxiety around eating. In severe cases, rapid weight loss occurs, further shrinking the mesenteric fat pad and worsening the obstruction. Some may also experience belching, constipation, or persistent digestive discomfort.
The complications of untreated SMAS can be serious. These include malnutrition risk, aspiration pneumonia, hypovolemic shock, and other life-threatening complications. Severe gastric outlet obstruction may require immediate intervention. Early recognition of these symptoms and proactive SMAS testing can prevent long-term harm and improve patient outcomes.
Diagnosis and Tests
Doctors diagnose SMAS using a combination of physical examination for diagnosis and medical history evaluation. The provider may perform a thorough check of abdominal pain, weight changes, and digestion issues. Imaging plays a central role in confirming the condition. Imaging tests for SMA syndrome include CT angiogram, endoscopic ultrasound, upper GI series, MRI scans, and X-rays to assess duodenum compression.
Differentiating SMAS from other conditions, like MALS or general gastrointestinal disorders, is essential. Accurate SMAS testing helps prevent misdiagnosis. Doctors rely on imaging tests for SMA syndrome and patient symptoms to decide whether conservative treatment for SMA syndrome or surgery is needed. Timely diagnosis reduces the risk of severe gastrointestinal obstruction and other complications.
Management and Treatment Options
Initial SMAS treatment is usually non-surgical. Nutritional support and meal replacement are vital for regaining the mesenteric fat pad. Patients may be advised to eat small, high-calorie meals or use total parenteral nutrition if oral intake is insufficient. Positioning techniques for symptom relief, like lying on the left side with knees pulled up, can reduce duodenum compression.
When conservative measures fail, surgical intervention options may include duodenojejunostomy, gastrojejunostomy, or relocating the duodenum to relieve compression. Dopamine antagonist medication such as Metoclopramide may help improve stomach motility. Recovery often depends on timely intervention and restoring normal small intestine function. Most patients regain full digestive capacity with proper SMAS treatment and recovery and prognosis is generally positive.
Recovery and Prognosis
Patients who receive SMAS treatment early usually recover fully. Rebuilding the mesenteric fat pad restores the duodenum’s normal function. Symptoms like abdominal pain, nausea, and early satiety often improve as weight stabilizes. Recovery requires careful monitoring, proper nutrition, and sometimes small intestine surgery. With timely care, patients can return to normal activity and avoid serious life-threatening complications.
SMA Syndrome vs. MALS
SMA Syndrome and Median Arcuate Ligament Syndrome (MALS) are often confused because both involve arterial compression. SMAS compresses the duodenum causing digestive disorder symptoms, while MALS compresses the celiac artery, causing different patterns of abdominal pain.
| Feature | SMAS | MALS |
|---|---|---|
| Cause | Duodenum compression by superior mesenteric artery | Celiac artery compression by ligament |
| Symptoms | Abdominal pain, vomiting, bloating | Post-meal pain, weight loss |
| Treatment | Conservative treatment for SMA syndrome, surgery if severe | Surgery to release ligament |
| Risk | Rapid weight loss, mesenteric fat pad loss | Less linked to weight changes |
| Diagnostics | CT angiogram, endoscopic ultrasound | Doppler ultrasound, angiography |
This comparison helps patients understand which condition affects them and why proper SMAS testing is critical.
Conclusion
Superior Mesenteric Artery Syndrome (SMAS) is a rare but treatable digestive disorder. Early recognition of abdominal pain, nausea and vomiting, early satiety, and rapid weight loss can prevent serious life-threatening complications. Both conservative treatment for SMA syndrome and surgical intervention options exist, and outcomes are generally positive with timely care.
Monitoring weight, using nutritional support and meal replacement, and following medical advice ensures recovery and restores normal small intestine function. Awareness and proper management can help patients live active, healthy lives despite SMAS.
FAQs
Q: What are the symptoms of SMAS?
A: Symptoms include abdominal pain, nausea, vomiting, bloating, early satiety, and rapid weight loss.
Q: Is there a cure for SMAS?
A: Yes, conservative treatment or surgery can relieve symptoms and restore normal digestion.
Q: What does SMAS stand for?
A: SMAS stands for Superior Mesenteric Artery Syndrome.
Q: What does SMAS pain feel like?
A: SMAS pain is cramping, upper abdominal discomfort, and worsens after eating.